 S
S
SoCal Eye – Diabetic Retinopathy in Long Beach
Diabetic Retinopathy is the leading cause of blindness among adults, retinopathy is the most common eye complication in diabetic patients, affecting more than 4.4 million Americans age 40 and older. Because its initial symptoms are very slight or even unnoticeable, diabetic retinopathy often goes undiagnosed. Once detected, it can be treated by laser surgery. SoCal Eye Ophthalmologists are diabetic eye specialists with extensive experience with Diabetic Retinopathy in Long Beach, Huntington Beach and Garden Grove. Treatment starts with a Comprehensive Eye Exam. Schedule an Appointment today at LAKEWOOD (562) 531-2020 | LOS ALAMITOS (562) 598-7728 or send us an Online Consultation Request
What is Diabetic Retinopathy?
Diabetic retinopathy is a general term for all disorders of the retina caused by diabetes. There are two major types of retinopathy: nonproliferative and proliferative.
Nonproliferative Retinopathy:
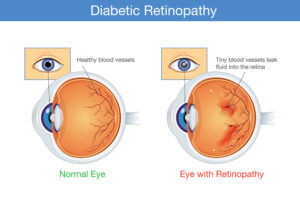
This is the most common form of retinopathy and is characterized by increased levels of blood sugar in diabetic patients causing damage to the tiny blood vessels in the retina, the part of the eye that captures and sends images to the brain. When these vessels become blocked or damaged, it can result in blood and fluid leakage leakage into the part of the eye where focusing occurs, the macula. When the macula swells with fluid, a condition called macular edema occurs and vision can decrease significantly.
In some people, retinopathy progresses to a more serious form called……
Proliferative Retinopathy:
In this form, the blood vessels are so damaged, they close off. In response, new blood vessels start growing in and around the retina. These new vessels are weak and can leak blood, blocking vision, which is a condition called vitreous hemorrhage. The new blood vessels can also cause scar tissue to grow. After the scar tissue shrinks, it can distort the retina or pull it out of place—causing what is called “retinal detachment.”
 Diabetic Retinopathy – Causes & Risk Factors:
Diabetic Retinopathy – Causes & Risk Factors:
Several factors influence whether you get retinopathy. They include blood sugar control, blood pressure levels, duration of diabetes, and genetics. The longer you have had diabetes, the more likely you are to have retinopathy. Almost everyone with type 1 diabetes, and many with type 2, will eventually have nonproliferative retinopathy. Serious proliferative retinopathy is far less common.
People who keep their blood sugar levels closer to normal are less likely to develop serious diabetic changes in the eye, as well as in the rest of the body.
Diabetic Retinopathy – Symptoms & Detection:
Symptoms:
Because its initial symptoms of Nonproliferative Retinopathy are very slight or even unnoticeable, the condition often goes undiagnosed until it’s too late. However, it can be detected during an annual comprehensive eye exam. When your eye doctor dilates your eyes, he or she can check your blood vessels for signs of damage. Fortunately, treatment is usually effective at stopping, and even reversing, vision loss.
In the more extreme forms of Proliferative Retinopathy, the retina can be severely damaged before there are any noticeable changes to the vision. People sometimes have no symptoms until it is too late to be treated.
Detection:
The Diabetic Retinopathy doctors at SoCal Eye can detect this condition by performing a comprehensive eye exam. The key is early detection and all diabetics should have their eyes examined at least yearly.
Treatment:
Blood Sugar Control:
Controlling blood sugar and blood pressure can stop vision loss. Dietary recommendations should be closely followed and adherence to prescribed drug regimens is vital. Good sugar control can reverse early capillary damage and can sometimes even bring some of your vision back. Controlling your blood pressure keeps your eye’s blood vessels healthy.
Pharmaceutical:
Anti-VEGF medication helps to reduce swelling of the macula, slowing vision loss and perhaps improving vision. This drug is given by injections (shots) in the eye. Steroid medication is another option to reduce macular swelling and is also given as injections in the eye.
Laser Surgery:
Laser surgery might be used to help seal off leaking blood vessels. This can reduce swelling of the retina. Laser surgery can also help shrink blood vessels and prevent them from growing again. Sometimes more than one treatment is needed.
- Photocoagulation: Procedure makes tiny spots on the retina with a special laser. These spots seal the blood vessels and stop them from growing and leaking.
- Scatter Photocoagulation: Procedure makes hundreds of spots in a polka-dot pattern on two or more occasions. Scatter photocoagulation reduces the risk of blindness from vitreous hemorrhage or detachment of the retina. Side effects of scatter photocoagulation are usually minor. They include several days of blurred vision after each treatment and possible loss of side (peripheral) vision.
- Focal Photocoagulation: Procedure aims the laser precisely at leaking blood vessels in the macula. This procedure assists the body in reabsorbing the fluid, which can aid in visual restoration.
SoCal Eye Consultation:
Diabetic Retinopathy is the most common diabetic eye disease and is a disorder of the retina. Initial symptoms are very slight or even unnoticeable, and it often goes undiagnosed. Early detection and treatment can reverse damage to the retina and vision loss can be avoided. If left untreated it can lead to vision loss and blindness. However, it can be detected during an annual comprehensive eye exam. SoCal Eye doctors are the Diabetic Retinopathy Specialists in Long Beach. Schedule an Appointment today at LAKEWOOD (562) 531-2020 | LOS ALAMITOS (562) 598-7728 or send us an Online Consultation Request



